Odoo for Healthcare Industry in USA: Hospital Management Software, Compliance & Billing
- April 20, 2026
- Posted by: Jaishree Jayabal Singh
- Categories: Blog, Odoo healthcare ERP USA
Why Hospitals Need Integrated Software
Healthcare delivery in the United States operates under intense pressure with strict regulations, rising operational costs, workforce shortages, and zero tolerance for clinical errors. In such an environment, disconnected systems create friction across departments, slow decision-making, and expose hospitals to financial and regulatory risks.
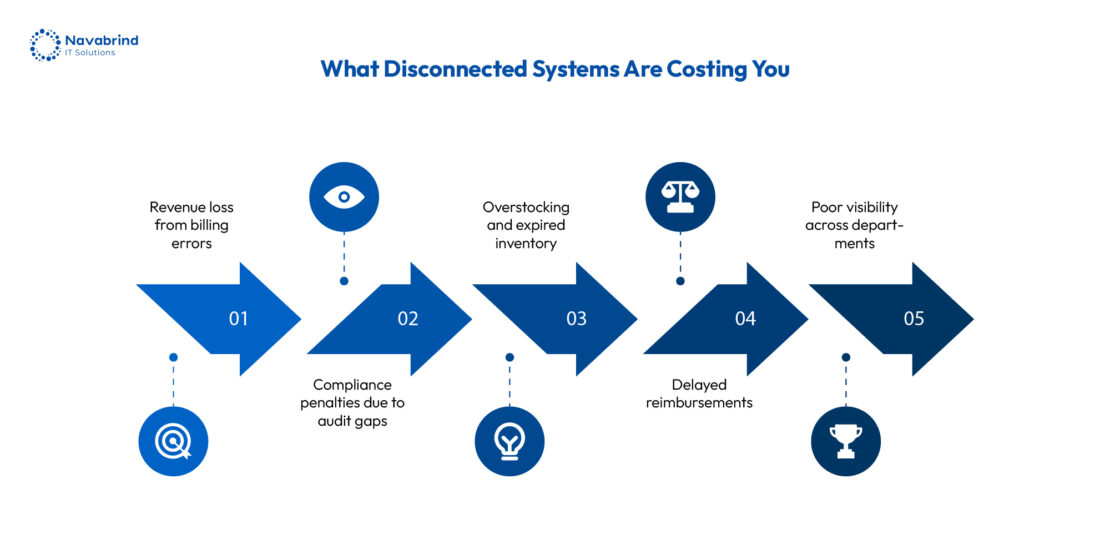
A fragmented technology landscape leads to serious consequences. Disparate tools across departments result in isolated data, inconsistent reporting, and gaps in visibility. This disconnect drives billing inaccuracies, delayed reimbursements, and audit challenges. Without a cohesive hospital management software, hospitals struggle to maintain financial discipline and regulatory alignment.
Hospitals that invest in an integrated ecosystem outperform their peers across key performance indicators. With centralized data and synchronized workflows, care teams gain better visibility into patient journeys, administrative teams reduce claim denials, and leadership gains actionable insights that influence margin improvement. A robust billing software for hospitals ensures accurate charge capture and faster revenue cycles, strengthening financial outcomes.
Regulatory demands continue to evolve, making compliance a non-negotiable priority. A well-aligned healthcare compliance software framework enables hospitals to maintain audit readiness, track policy adherence, and reduce exposure to penalties. When compliance, billing, and operations function within one connected environment, hospitals operate with greater control and confidence.
Operational efficiency extends beyond patient care. Procurement and inventory management play a critical role in cost containment. A reliable hospital supply chain management software combined with hospital inventory management software ensures optimal stock levels, reduces wastage, and prevents critical shortages. This level of coordination enhances service delivery without inflating operational costs.
Contractual oversight is another area where fragmentation creates risk. Managing vendor agreements, service contracts, and compliance obligations through contract management software for hospitals ensures accountability, minimizes disputes, and safeguards financial interests.
This guide is designed for decision-makers who influence hospital performance and growth:
- Hospital administrators focused on operational excellence
- CFOs responsible for financial performance and cost control
- IT directors evaluating scalable digital infrastructure
- Procurement teams managing vendor relationships and supply continuity
Hospital Management Software: The Digital Backbone
A high-performing healthcare system depends on a connected digital foundation. Hospital management software brings clinical, administrative, and financial operations into one coordinated environment, replacing disconnected tools with a cohesive framework that supports accuracy, accountability, and speed across departments.
At its foundation, hospital management software includes critical modules that support end-to-end hospital operations:
- Patient records with complete medical histories and treatment tracking
- Appointment scheduling that aligns clinical staff, resources, and patient flow
- Billing software for hospital to manage charge capture, claims processing, and reimbursements
- Laboratory management for diagnostics, reporting, and test workflows
- Pharmacy operations with medication tracking and dispensing control
- Human resource management to handle staffing, payroll, and compliance requirements
Each module contributes to a connected ecosystem, enabling hospitals to operate with greater coordination and financial control.
- A key decision in adopting hospital management software lies in choosing between on-premise infrastructure and cloud-based deployment. Traditional on-premise systems demand heavy capital investment, ongoing maintenance, and internal IT dependency. In contrast, cloud-based models offer cost predictability, faster deployment cycles, and the flexibility to scale across expanding hospital networks. Security protocols within cloud environments now meet stringent healthcare standards, making them a reliable choice for handling sensitive patient and financial data.
- Cloud-enabled hospital management software transforms how hospitals operate across multiple locations. Leadership teams gain access to live operational data, finance teams track revenue performance without delays, and clinicians view patient records across facilities without disruption. This level of access strengthens coordination, reduces duplication, and supports informed decision-making at scale.
- Selecting the right system requires careful evaluation of critical capabilities. Interoperability remains a top priority, with standards such as HL7 and FHIR ensuring smooth data exchange between systems. Reliable vendor support influences implementation success and long-term system stability. Uptime commitments defined through service-level agreements protect hospitals from operational downtime that can impact patient care and revenue cycles.
- Hospitals adopting cloud-based hospital management software report measurable gains. These include reduced billing discrepancies through integrated billing software for hospital, faster claims processing, improved compliance tracking through aligned healthcare compliance software, and tighter cost control supported by connected hospital supply chain management software and hospital inventory management software.
This digital backbone positions hospitals to operate with clarity, financial discipline, and operational resilience turning technology investment into measurable business outcomes.
Healthcare Compliance & Risk:
- Regulatory adherence and risk control operate as two sides of the same discipline. Treating them as isolated functions creates blind spots that expose hospitals to financial penalties, legal disputes, and operational disruption. A connected framework anchored by healthcare compliance software brings these functions together, replacing fragmented checklists with a system that tracks, monitors, and enforces accountability across the organization.
- The U.S. healthcare landscape demands strict adherence to multiple regulatory bodies. HIPAA governs patient data privacy and security, The Joint Commission sets accreditation standards tied to quality and safety, and Centers for Medicare & Medicaid Services (CMS) enforces reimbursement and reporting requirements. State-level mandates add another layer of oversight, increasing the complexity hospitals must manage on a daily basis. Without a coordinated system, maintaining alignment across these frameworks becomes resource-intensive and error-prone.
- A well-implemented healthcare compliance software platform automates critical processes that would otherwise consume significant administrative effort. Audit preparation becomes systematic with documented trails and evidence tracking. Staff training programs are monitored for completion and effectiveness. Incident reporting captures deviations, enabling leadership to act on risks before they escalate. This structured approach reduces reliance on scattered documentation and strengthens audit readiness.
- Risk management within hospitals requires a shift from reactive reporting to proactive identification. Integrated systems evaluate patterns across clinical, operational, and financial data to flag potential issues early. When paired with hospital management software, risk indicators as repeated billing inconsistencies or inventory discrepancies that can be identified and addressed before they impact patient care or revenue. This approach transforms risk management from a defensive activity into a continuous monitoring discipline.
- The true strength of an integrated environment lies in shared data across compliance and risk modules. Insights from incident reports feed into compliance audits. Training gaps identified through compliance reviews inform risk mitigation strategies. This closed feedback loop ensures that lessons learned translate into operational improvements, strengthening governance across departments.
- The financial impact of non-compliance is significant. HIPAA violations can result in penalties ranging from $100 to $50,000 per violation, with annual caps reaching $1.5 million per category. Non-compliance with CMS requirements can lead to reimbursement denials and exclusion from federal programs. Legal actions and reputational damage further compound these losses, affecting patient trust and long-term revenue stability.
- Integration with clinical and administrative systems completes the compliance framework. When healthcare compliance software connects with EHR platforms, hospitals gain visibility into patient data handling and access controls. Integration with HR systems ensures that staff certifications, training records, and policy acknowledgments remain up to date. Combined with hospital management software, this interconnected approach provides leadership with a unified view of compliance status, risk exposure, and corrective actions.
Hospitals that align compliance and risk within a single ecosystem gain stronger governance, reduced exposure to penalties, and a measurable improvement in operational reliability.
Billing Software for Hospitals: Turning Revenue Cycles into a Competitive Asset
Financial stability in healthcare hinges on how well revenue flows from patient intake to final reimbursement. Billing software for hospital environments transforms revenue cycle management (RCM) from a back-office task into a performance engine that safeguards cash flow, reduces leakage, and strengthens margin control. At its foundation, RCM covers the full financial journey, patient registration, insurance verification, charge capture, coding, claims submission, payment posting, and follow-ups. Gaps at any stage create delays, lost revenue, and administrative burden. When aligned with hospital management software, this cycle becomes tightly coordinated, giving finance teams visibility and control over each transaction. Hospitals face recurring billing breakdowns that erode revenue. Coding inaccuracies lead to claim rejections. Incomplete documentation triggers payer queries. Delayed submissions extend reimbursement timelines. High denial volumes consume staff time and increase operational costs. Without a connected system, these issues compound, limiting financial predictability.
A high-performing billing software for hospital setup introduces capabilities that elevate revenue performance:
- AI-assisted coding that improves accuracy across ICD-10 and CPT classifications
- Eligibility verification at the point of registration to prevent claim rejection
- Denial management workflows that identify root causes and accelerate resolution
- Charge capture validation to prevent missed or under-coded services
These features convert billing into a controlled, data-driven function that supports consistent revenue capture.
Integration plays a critical role in maximizing billing efficiency. When billing software for hospital connects with EHR systems, clinical documentation flows into coding without gaps. Integration with insurance payer networks streamlines claim submission and status tracking, reducing turnaround time and administrative workload. This interconnected flow minimizes friction across departments and ensures that financial data reflects clinical activity accurately. Compliance remains central to revenue operations. Adherence to ICD-10 and CPT standards is mandatory for accurate coding and reimbursement. A reliable system maintains audit trails for each transaction, supporting transparency during payer reviews and regulatory audits. When aligned with healthcare compliance software, billing operations remain consistent with regulatory expectations, reducing exposure to penalties and disputes.
Hospitals track performance through key financial indicators that reflect billing effectiveness:
- Clean claim rate, indicating the percentage of claims accepted on first submission
- Days in accounts receivable (AR), measuring how quickly payments are collected
- Denial rate, highlighting the volume of rejected or disputed claims
Improvement across these metrics signals stronger revenue control and operational discipline. When integrated with hospital management software, billing software for hospital shifts from a reactive process to a revenue-driving function. Hospitals gain faster reimbursements, reduced claim rework, and improved financial forecasting by turning billing into a competitive advantage rather than an operational burden.
Hospital Supply Chain & Inventory Management: Ending the Stockout Crisis
The pandemic revealed how fragile hospital supply chains can become under pressure. Stockouts, delayed procurement, and uncontrolled inventory levels disrupted care delivery and increased operational costs. A connected approach using hospital supply chain management software and hospital inventory management software transforms this critical function into a controlled, data-driven system that protects both patient care and financial performance. Inefficiencies within supply chains carry hidden costs. Excess inventory leads to expired products and wasted spend. Emergency procurement drives up purchase prices and strains vendor relationships. Delays in material availability impact treatment timelines and patient satisfaction. Without visibility and coordination, hospitals absorb these losses across departments without a clear path to correction.
A robust hospital supply chain management software platform introduces discipline across procurement and vendor operations. It enables centralized vendor management, tracks supplier performance, and standardizes purchasing workflows. Demand forecasting based on historical usage patterns allows procurement teams to plan inventory levels with confidence, reducing reliance on last-minute purchasing decisions. This level of control stabilizes costs and improves supply reliability. On the operational side, hospital inventory management software ensures accurate tracking of medical supplies across locations. Hospitals gain visibility into stock levels, movement, and usage patterns. Expiry tracking reduces the risk of using outdated materials, while par-level automation maintains optimal stock thresholds without overstocking. This balance minimizes waste and ensures that critical items remain available when needed.
Integration with clinical systems strengthens inventory accuracy. Consumption data captured at the point of care feeds directly into inventory records, reflecting actual usage rather than estimates. When aligned with hospital management software, this connection ensures that supply chain decisions are based on clinical demand, not assumptions. The result is tighter coordination between care delivery and resource availability. Technology advancements are reshaping how hospitals manage inventory. RFID and IoT-enabled tracking systems provide continuous monitoring of high-value and high-risk items. These tools improve traceability, reduce loss, and enhance accountability across departments. Hospitals adopting these technologies gain a measurable edge in inventory control and operational transparency.
Sustainability has become a key consideration in healthcare operations. Reducing expired stock and limiting over-ordering lowers environmental impact and supports cost control. With hospital supply chain management software and hospital inventory management software, hospitals align operational efficiency with responsible resource utilization. When supply chain and inventory systems operate within a connected ecosystem, hospitals eliminate stockout risks, reduce waste, and strengthen financial discipline. This transformation turns supply management from a reactive function into a predictable, value-driven operation.
Contract Management Software for Hospitals: The Overlooked Saving Lever
Hospitals manage an extensive network of agreements that influence revenue, compliance, and operational stability. Payer contracts, vendor SLAs, physician employment terms, and service agreements create a complex web of obligations. Without a centralized system, this contract sprawl leads to missed renewals, inconsistent terms, and lost revenue opportunities. Contract management software for hospitals brings order to this complexity and converts contract oversight into a measurable financial advantage.
Uncontrolled contract environments create hidden risks. Payer agreements may contain reimbursement clauses that go underutilized. Vendor contracts may include pricing terms that are not enforced. Physician agreements may carry compliance obligations that require continuous monitoring. When these documents are scattered across departments, hospitals lose visibility and control.
A well-implemented contract management software for hospitals platform introduces discipline across the contract lifecycle. Version control ensures that teams work with current agreements. Expiry alerts prevent missed renewals and renegotiation windows. Clause libraries standardize contract language, reducing legal ambiguity and strengthening consistency across agreements. This structured approach reduces administrative overhead and enhances accountability.
Compliance requirements add another layer of complexity. Regulations such as the Stark Law and the Anti-Kickback Statute demand strict adherence to contractual terms, especially in physician and vendor relationships. Inaccurate payer contracts can lead to billing discrepancies and audit exposure. When aligned with healthcare compliance software, contract management systems help hospitals maintain regulatory alignment and reduce legal risk.
Integration across departments strengthens contract governance. When contract management software for hospitals connects with procurement systems, vendor agreements align with purchasing activities and pricing terms. Integration with legal workflows ensures that contract reviews, approvals, and updates follow a consistent process. Within a broader hospital management software ecosystem, contract data becomes accessible to finance, compliance, and operations teams, improving coordination and decision-making.
The financial impact of effective contract management is substantial. Hospitals can recover revenue from under-billed payer contracts by aligning billing practices with negotiated terms. Enforced vendor pricing reduces procurement costs. Timely renewals and renegotiations protect margins and improve financial predictability. These gains position contract management as a direct contributor to profitability rather than an administrative function.
Selecting the right platform requires careful evaluation. Healthcare-focused solutions offer alignment with regulatory requirements and payer contract complexities. General contract lifecycle management (CLM) platforms provide flexibility across industries. Hospitals must assess their operational priorities, compliance requirements, and integration needs before making a decision.
When deployed within a connected ecosystem, contract management software for hospitals transforms contract oversight into a controlled, revenue-focused discipline unlocking value that often remains hidden within complex agreements.
ERP for Medical Device Manufacturers: A Different Set of Demands
Medical device manufacturers operate under strict regulatory oversight, where product quality, traceability, and documentation determine market access. Generic ERP platforms fail to meet these demands due to limited support for regulatory controls and quality processes. An ERP aligned with healthcare manufacturing requirements bridges this gap, ensuring compliance, operational control, and product integrity from design to distribution.
Regulatory frameworks such as FDA 21 CFR Part 11, ISO 13485, and UDI requirements define how data is recorded, stored, and audited. These standards require electronic records with validation, controlled access, and complete traceability. Without a system designed for these mandates, manufacturers face audit risks, delayed approvals, and restricted market entry.
A robust medical device ERP software environment includes critical modules that support manufacturing and compliance:
- Bill of Materials (BOM) management for accurate product configuration
- Lot and serial traceability to track components and finished devices across the lifecycle
- CAPA (Corrective and Preventive Actions) to manage quality incidents and corrective workflows
- Device History Records (DHR) to maintain detailed production and quality documentation
These capabilities ensure that manufacturers maintain full visibility into product history and quality performance.
Quality management integration plays a central role in device manufacturing. Non-conformance tracking identifies deviations in production or materials. Audit management ensures readiness for regulatory inspections. Supplier quality management evaluates vendor performance and material consistency. When these functions operate within the ERP environment, manufacturers maintain tighter control over product standards and regulatory expectations.
Regulatory submissions demand detailed documentation and traceability. ERP systems support the preparation of 510(k) submissions for the U.S. market and help manufacturers align with EU MDR requirements. Centralized documentation ensures that product data, testing records, and validation reports remain accessible and consistent during submission processes.
Deployment models influence validation and compliance readiness. Cloud-based ERP solutions reduce infrastructure overhead and support scalability, though they require validation to meet regulatory standards. On-premise systems offer greater control over validation environments but demand higher maintenance and resource investment. Manufacturers must evaluate these options based on compliance requirements and operational priorities.
On the production floor, ERP systems work alongside Manufacturing Execution Systems (MES) to maintain process control. ERP manages planning, inventory, and compliance data, while MES tracks production activities in real time, ensuring adherence to defined processes. This integration connects planning with execution, improving accuracy and traceability across manufacturing operations.
For organizations operating across healthcare delivery and manufacturing, alignment between ERP and hospital management software strengthens supply chain coordination, quality control, and compliance tracking. This connected approach ensures that medical devices meet regulatory standards while supporting efficient distribution to healthcare providers.
Medical Clinic Management Systems: Right-Sized Solutions for Small Practices
Not every healthcare provider operates at hospital scale. Clinics, general practitioners, and specialty practices require systems that match their pace, patient volume, and operational scope. A focused approach using hospital management software adapted for clinics delivers control without unnecessary complexity, helping smaller practices maintain quality care and financial stability.
Where Clinic Needs Diverge from Hospital Systems
Clinics operate with lean teams, shorter patient cycles, and tighter budgets. Large-scale hospital platforms introduce layers of functionality that may not align with daily workflows in a clinic setting. What matters here is speed, usability, and cost control by ensuring that staff can manage appointments, records, and billing without operational friction.
Core Features That Support Daily Operations
A well-designed clinic system includes capabilities that directly impact patient experience and practice efficiency:
- Appointment scheduling that reduces wait times and improves patient flow
- Patient portals that allow access to records, prescriptions, and communication
- E-prescribing to streamline medication management and reduce errors
- SOAP notes for consistent clinical documentation
These features ensure that care delivery and administrative tasks remain aligned within a single environment.
Revenue management remains critical for clinics. A reliable billing software for hospitals adapted for smaller practices handles insurance verification, claim submission, and payment tracking. This reduces administrative workload and improves reimbursement timelines, allowing practitioners to focus on patient care rather than financial follow-ups.
Virtual consultations have become a standard part of healthcare delivery. Clinics require systems that support telemedicine, enabling remote consultations, digital prescriptions, and follow-up care. This expands patient reach and ensures continuity of care without physical visits.
Cloud deployment offers flexibility and cost predictability for clinics. Systems aligned with healthcare compliance software standards ensure HIPAA compliance, secure patient data handling, and audit readiness. Transparent pricing models help clinics plan expenses without unexpected costs, making technology adoption more sustainable.
Choosing the wrong platform can create long-term challenges. Clinics should watch for:
- Hidden fees that increase total cost over time
- Limited customer support that delays issue resolution
- Weak interoperability that restricts integration with labs, pharmacies, or insurance systems
Selecting a system that aligns with operational needs, compliance requirements, and financial goals ensures that clinics gain value without unnecessary complexity. For small practices, the right digital foundation supports growth, improves patient engagement, and strengthens revenue control without the overhead associated with large hospital systems.
How to Build an Integrated Healthcare Software Stack
Healthcare organizations cannot rely on disconnected applications without creating operational gaps. Standalone tools introduce duplicate data entry, inconsistent reporting, and delays in decision-making. A connected ecosystem anchored by hospital management software aligns clinical, financial, and administrative functions into one coordinated framework that supports accuracy and accountability.
The Integration Imperative
Disconnected systems create friction across departments. Patient data remains isolated, billing teams lack visibility into clinical documentation, and compliance tracking becomes fragmented. Integration resolves these gaps by ensuring that information flows across systems without disruption. When hospital management software connects with billing software for hospitals, healthcare compliance software, and operational tools, hospitals gain a unified view of performance and risk.
Recommended Integration Sequence:
A phased approach ensures stability and measurable progress:
- Start with hospital management software to centralize patient, clinical, and administrative data
- Integrate billing software for hospital to align revenue cycles with clinical activity
- Introduce healthcare compliance software to track regulatory adherence and audit readiness
- Add hospital supply chain management software and hospital inventory management software to control procurement and stock levels
- Implement contract management software for hospitals to manage agreements and financial obligations
This sequence builds a strong foundation before expanding into supporting functions.
API Standards That Enable Interoperability
Standards such as HL7 and FHIR enable healthcare systems to exchange data in a consistent format. REST-based APIs support communication between platforms, allowing hospitals to connect EHRs, billing systems, and compliance tools without disruption. These standards ensure that data remains accessible and usable across the organization.
Build vs. Buy vs. Best-of-Breed vs. Single-Vendor Suite
Hospitals must evaluate different approaches based on their operational goals:
- Build: Offers control over functionality but requires significant development effort and ongoing maintenance
- Buy: Provides faster deployment with pre-configured features
- Best-of-breed: Combines specialized tools for each function, offering flexibility with integration complexity
- Single-vendor suite: Delivers a connected ecosystem with fewer integration challenges and consistent user experience
Selecting the right approach depends on budget, technical capability, and long-term scalability requirements.
Cloud-First Architecture Considerations
Cloud-based environments support scalability, remote access, and reduced infrastructure overhead. Hospitals can expand operations across locations without heavy capital investment. Security frameworks within cloud platforms meet healthcare standards, ensuring patient data protection and regulatory compliance. This approach supports growth while maintaining operational control.
Change Management: The Human Side of Implementation
Technology adoption succeeds when people align with the system. Staff training, stakeholder involvement, and process alignment play a critical role in implementation success. Clear communication of benefits, phased rollouts, and continuous support help teams adapt to new workflows. Without this focus, even the most advanced systems fail to deliver expected outcomes.
A well-integrated healthcare software stack transforms operations into a connected, data-driven environment. Hospitals gain visibility, reduce inefficiencies, and strengthen financial and compliance performance turning technology investment into measurable results.
Healthcare organizations can no longer rely on disconnected systems to manage clinical care, compliance, and financial performance. This guide has outlined how hospital management software, billing software for hospitals, healthcare compliance software, hospital supply chain management software, hospital inventory management software, and contract management software for hospitals work together to form a connected digital ecosystem. Each layer plays a critical role in improving visibility, reducing operational gaps, and strengthening revenue outcomes.
A 3-Step Action Framework:
1. Audit Your Current Systems
Evaluate existing tools across clinical, financial, compliance, and operational functions. Identify inefficiencies, duplicate processes, and data silos that limit performance.
2. Identify Critical Gaps
Pinpoint where integration is missing whether in billing accuracy, compliance tracking, inventory control, or contract oversight. Focus on areas that directly impact revenue and risk.
3. Prioritize Based on ROI
Invest in solutions that deliver measurable impact. Start with hospital management software as the foundation, then expand into billing software for hospital, healthcare compliance software, and operational systems to build a connected environment.
Take the Next Step
If your organization is looking to strengthen operational control and financial performance, now is the time to act. Explore solution capabilities, evaluate system fit, and move forward with a platform that aligns with your growth objectives. Request a personalized demo to understand how an integrated approach can transform your healthcare operations.
Suggested Reads
- Hospital Management Software: Key Features and Selection Guide
- Healthcare Compliance Software: Managing Risk and Regulatory Alignment
- Billing Software for Hospital: Improving Revenue Cycle Performance
- Hospital Supply Chain Management Software: Reducing Costs and Waste
- Contract Management Software for Hospitals: Strengthening Financial Control
Frequently Asked Questions
1. What is hospital management software and how does cloud based hospital management software improve operations?
Hospital management software connects clinical, administrative, and financial workflows into one system, reducing data gaps and improving coordination. A cloud based hospital management software setup enables access to patient records, billing data, and operational insights across multiple locations. This supports faster decision-making, stronger collaboration, and better control over hospital performance.
2.How does healthcare compliance software and healthcare compliance management software help hospitals stay compliant?
Healthcare compliance software and healthcare compliance management software automate audit tracking, staff training, policy management, and incident reporting. These systems ensure adherence to regulations such as HIPAA and CMS guidelines. When integrated with hospital risk management software, they help identify risks early and maintain continuous compliance across departments.
3.Why is billing software for hospitals critical for revenue cycle management?
Billing software for hospitals ensures accurate coding, faster claims submission, and reduced denial rates. When integrated with hospital management software, it aligns clinical documentation with financial workflows, improving reimbursement timelines. This reduces revenue leakage and strengthens financial stability.
4.How do hospital supply chain management software and hospital inventory management software improve efficiency?
Hospital supply chain management software manages procurement, vendor relationships, and demand forecasting. Hospital inventory management software tracks stock levels, expiry dates, and usage patterns. Together, they reduce wastage, prevent stockouts, and ensure that hospitals maintain optimal inventory levels aligned with patient care needs.
5. What role does contract management software for hospitals play in financial performance?
Contract management software for hospitals tracks payer agreements, vendor contracts, and physician terms. It ensures pricing accuracy, monitors renewals, and enforces contract conditions. When combined with billing software for hospital, it helps recover lost revenue and improves margin control.
6. Why do medical device manufacturers need ERP for medical device manufacturers and medical device erp software?
ERP for medical device manufacturers and medical device erp software support regulatory compliance, product traceability, and quality management. These systems manage BOMs, lot tracking, CAPA processes, and documentation required for FDA and ISO standards. They ensure that manufacturers maintain control over production and meet regulatory requirements.
7. How does a medical clinic management system differ from hospital management software?
appointment scheduling, patient records, e-prescribing, and billing. In contrast, hospital management software handles larger, multi-department operations. Clinics benefit from simpler workflows, while hospitals require broader integration with healthcare compliance software, hospital inventory management software, and other systems.
Schedule a conversation with us now!
written by

Jaishree Jayabal Singh
Program Manager
Jaishree Jayabal Singh is a seasoned Program Manager with over a decade of experience leading client‑critical technology projects. She specializes in managing complex, time‑sensitive deliverables built on platforms such as Odoo, Magento, Akeneo, Pimcore, and WordPress, ensuring on‑time delivery, scope adherence, and high‑quality outcomes. Her expertise spans multiple industries, including manufacturing, electronics, retail, healthcare, and others, where she has successfully driven digital and system modernization programs. Jaishree has worked with clients across geographies, including the United States, Canada, the UK, the Netherlands, Belgium, and India. As a certified Akeneo and Odoo consultant, she combines technical knowledge with strong program‑management skills to align technology roadmaps with strategic business objectives.
Related Articles
-
Post
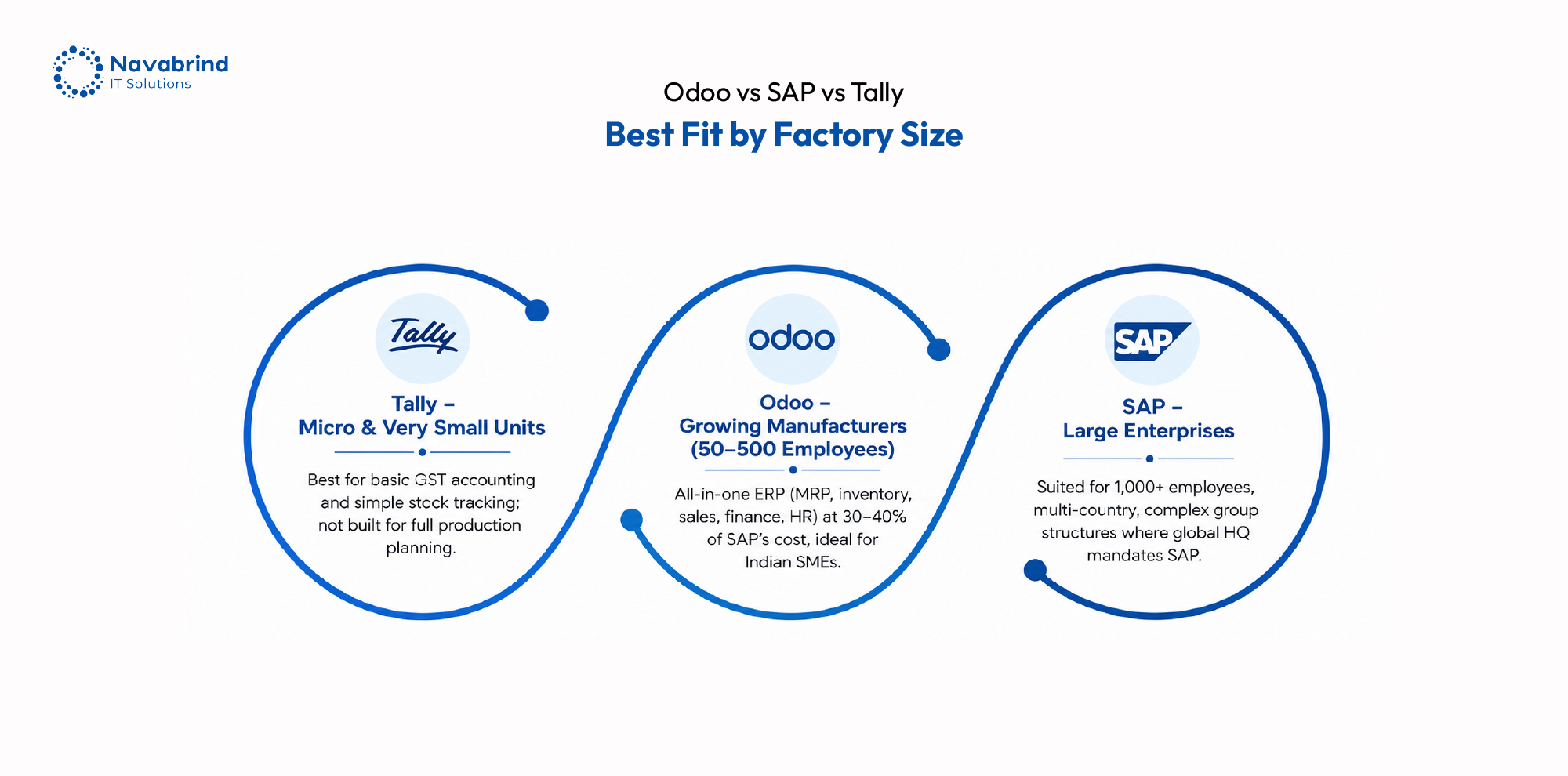
Odoo vs SAP vs Tally for Indian Manufacturing: Which Fits Your Factory?
Odoo vs SAP vs Tally for Indian Manufacturing: Which Fits Your Factory? June 3, 2026 Posted by: Abinay Subramaniam P Categories: Blog, ERP Software, Manufacturing ERP, Odoo ERP No Comments Indian manufacturers are no longer choosing ERP software based on brand recognition alone. The decision now shapes production control, inventory visibility, vendor coordination, compliance management, -
Post
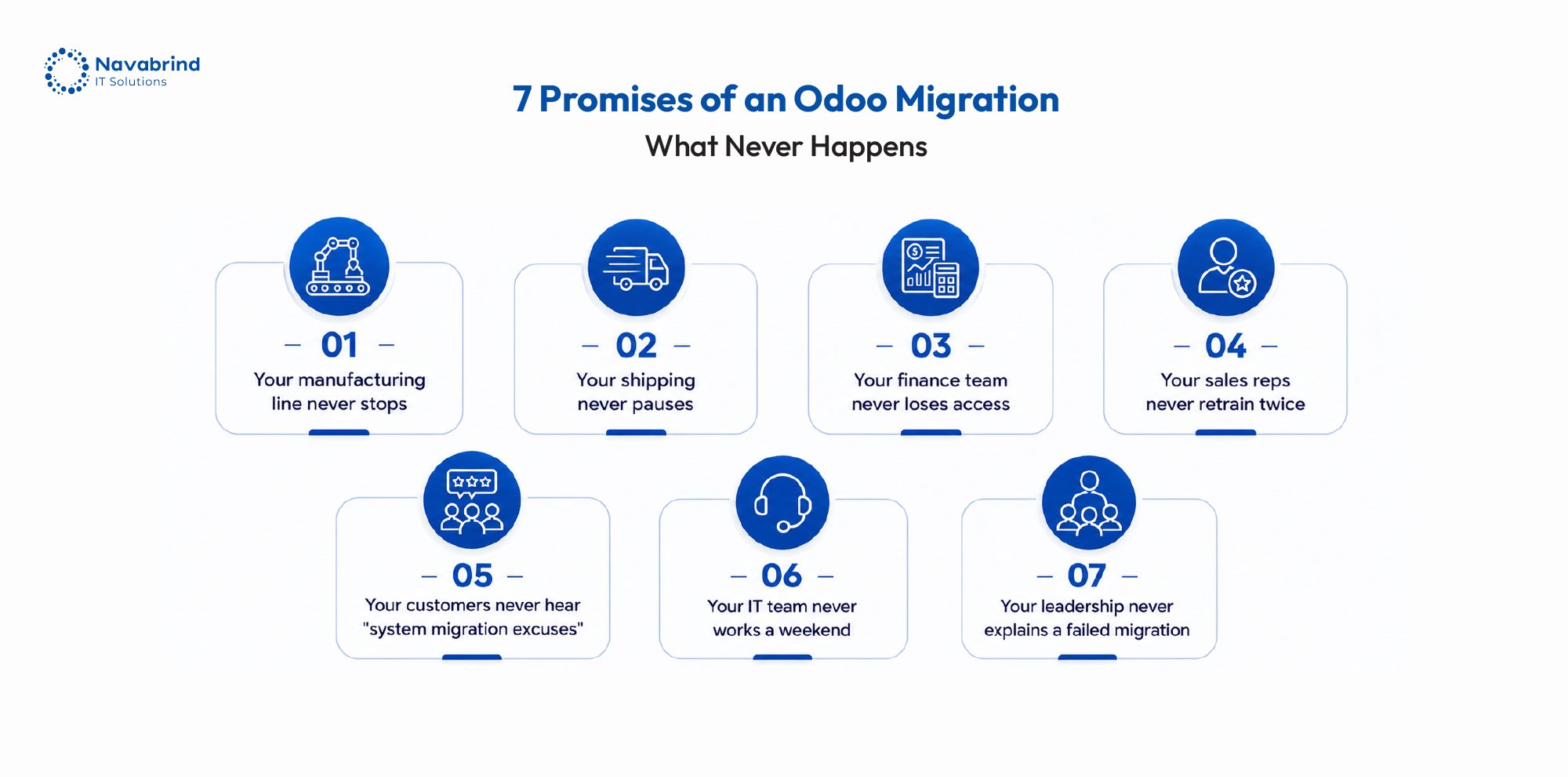
How Mid-Size US Companies Are Migrating from Oracle NetSuite to Odoo Without Disrupting Operations
How Mid-Size US Companies Are Migrating from Oracle NetSuite to Odoo Without Disrupting Operations June 2, 2026 Posted by: Lillian D Costa Categories: Blog, ERP Migration, Odoo ERP No Comments NetSuite earned early trust as a growth-stage ERP. Today, rising subscription costs, layered customizations, and operational friction are forcing mid-size companies to reconsider that investment. -
Post
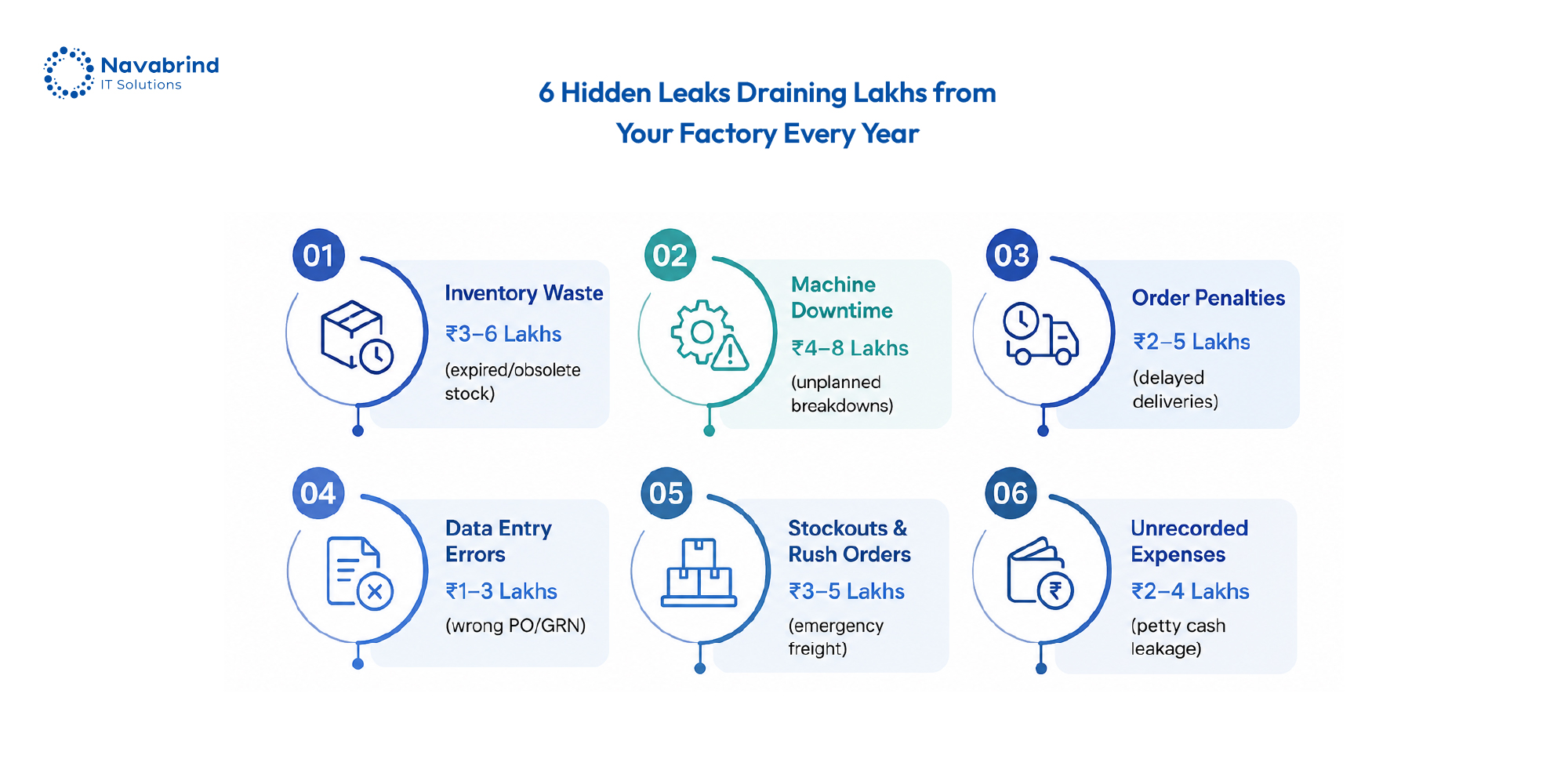
Why Indian Manufacturers Are Losing Lakhs Every Year Without ERP Software
Why Indian Manufacturers Are Losing Lakhs Every Year Without ERP Software June 1, 2026 Posted by: Jaishree Jayabal Singh Categories: Blog, Odoo ERP for Manufacturing No Comments Indian manufacturers are under pressure from rising material costs, tighter delivery timelines, GST compliance demands, machine downtime, and unpredictable supply chains. Yet many factories still depend on disconnected
written by

Jaishree Jayabal Singh
Program Manager
Jaishree Jayabal Singh is a seasoned Program Manager with over a decade of experience leading client‑critical technology projects. She specializes in managing complex, time‑sensitive deliverables built on platforms such as Odoo, Magento, Akeneo, Pimcore, and WordPress, ensuring on‑time delivery, scope adherence, and high‑quality outcomes. Her expertise spans multiple industries, including manufacturing, electronics, retail, healthcare, and others, where she has successfully driven digital and system modernization programs. Jaishree has worked with clients across geographies, including the United States, Canada, the UK, the Netherlands, Belgium, and India. As a certified Akeneo and Odoo consultant, she combines technical knowledge with strong program‑management skills to align technology roadmaps with strategic business objectives.
How can we help you?
Get in touch with a solutions consultant that can share best practices and help solve specific challenges.